Shoulder labral tears can be quite difficult to diagnosis and manage. These injuries are typically found in athletic populations in sports that require frequent overhead movements. It is important to consult a health professional such as a physical therapist and sports physician if you suspect a shoulder injury. The guide below detail what a labral tear is and how it might be managed.
ANATOMY
The glenoid labrum is a cartilage-like structure which sits within the shoulder joint (glenohumeral fossa). It serves several purposes which include:
- Improving the stability of the shoulder joint by deepening the socket
- Providing feedback to the body about the shoulder’s movement
- Acts as an attachment site for ligaments and muscles (such as the biceps)
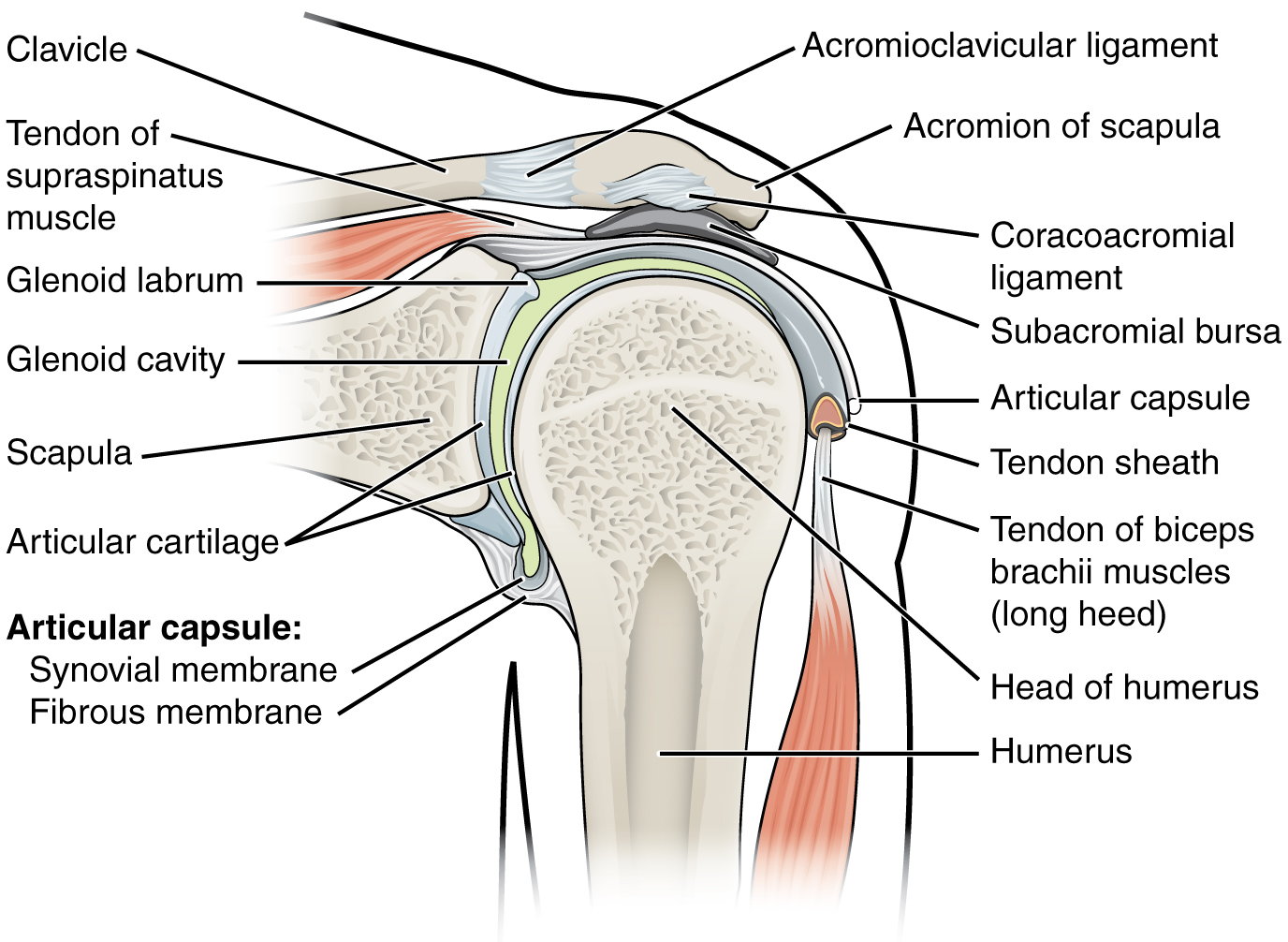
Image 1. Anatomical image of the shoulder and glenoid labrum.Source: https://upload.wikimedia.org/wikipedia/commons/6/67/914_Shoulder_Joint.jpg
Labral injuries and tears
Overview
A labral injury to the shoulder typically presents as a tear in varying locations of the glenoid labrum. Unlike labral tears to the hip, the glenoid labrum is much more complex. As there are many structures and attachments to the labrum, there are a variety of ways the injury can present.
Some common classifications of a labral injury include:
- SLAP lesion: SLAP stands for superior labrum anterior to posterior. This means that the location of the injury extends from the front of the structure and up towards the back. As seen in image 1, the biceps tendon is typically involved in a SLAP lesion because of its attachment location on the labrum. Additionally, there are a separate 4 sub-classifications of SLAP lesions
- Bankart lesion: This injury usually occurs because of repeated shoulder anterior dislocations. This can result in the damage to the anterior or front part of the labrum.
- Reverse-bankart lesion: Also known as a posterior labral tear, this injury affects the rear and lower ends of the labrum. The management of these labrum injuries will depend on the classification, severity of the injury and the stability of the shoulder. Consulting a relevant health professional such as a sports physician, physical therapist and specialist is recommended.
Mechanism of injury
The mechanism of injury refers to the type of actions or events that lead to a specific type of injury. Given that the shoulder joint is both the most mobile but unstable joint in the body, there are various points of vulnerabilities. Consequently, there are a few different types of mechanisms of injuries for labral tears which include:
- Repetitive overhead movements such as throwing or serving tennis balls
- Compressive forces acting on the labrum (e.g. falling on an outstretched hand, motor vehicle accidents)
- High impact pulling forces such as lifting heavy objects
- Repeated bouts of shoulder instability
- Single-event or repetitive shoulder dislocations
These types of injuries are particularly common in athletes such as weightlifters, tennis players, baseballers, swimmers etc. Any sport or activity which may require the athlete to use their shoulder in these provocative positions can lead to labral tears.
Signs and symptoms
The signs and symptoms of a labral tear will usually depend on the location and severity of the injury. More severe tears, particularly those who underwent trauma, may become more symptomatic. Whereas minor labral tears may have mild or even no symptoms. Generally, those with labral injuries may experience:
- Feeling of a “dead arm” – the inability to produce power through movement such as throwing
- Reduce shoulder mobility and movement
- Clicking, grinding and popping of the shoulder
- Pain with movements such as pushing or overhead
- Shoulder instability
Diagnosis
As with all musculoskeletal injuries, consulting a health professional such as physical therapist or physician will assist with diagnosis. Thorough questioning and a physical assessment will be conducted to determine the possibility of a labral tear. Information such as the mechanism of injury, symptoms, range of motion and specific tests will be of interest. Depending on the assessment, additional investigations such as x-rays or an MRI may be required to confirm the diagnosis.
Clinically, the O’Brien’s test is commonly used by physical therapists to determine the presence of a SLAP lesion. A therapist will need to be present when performing this diagnostic test. However, a positive test will not guarantee the diagnosis of a labral injury. An example of this test can be seen below:
However, one less commonly used measurement that can be performed by yourself is the Bear-Hug Test. If pain is triggered during the test, this may suggest that the labrum has been involved in the injury. However, the Bear-Hug test is not completely accurate.
Once again, for an appropriate diagnosis, these physical tests alone will not be able to accurately diagnose your shoulder condition. Seeing a relevant health professional is advised.
Management of Labral Tears
As mentioned, the management of labral tears will require an expert opinion from relevant healthcare professionals such as a sports physician and physical therapist. A comprehensive diagnosis and physical examination should be performed to determine the best course of action. Additionally, a specialist such as an orthopaedic surgeon may be referred to where necessary.
In some cases, physical therapy and rehabilitation may be trialled before more invasive treatment such as surgery. Anecdotally, candidates with less traumatic labral injuries will tend to yield better outcomes. Interestingly, it is also important to be aware that minor labral tears that are asymptomatic generally do not require treatment.
Physical Therapy
Currently, there is a lack of substantial evidence supporting physical therapy for managing shoulder labral tear particularly in more traumatic lesions such as Bankart and Reverse-Bankart Lesions. Typically, physical therapy will be recommended after surgical intervention for such injuries. Interestingly, there is more research supporting physical therapy as a first-line treatment for SLAP lesions.
There are several considerations when it comes to conservative management such as:
- Using ice and medication to manage the pain
- Physical therapy and rehabilitation focussing on strength, motor control and mobility
- Activity modifications through daily activities
- Taking a break from certain activities such as sport or work
A 2010 study focussed on identifying the effectiveness of physical therapy for SLAP lesions. They were able to show that consistent rehabilitation was able to improve pain, function, and quality of life. Also, around 50% of those subjects were able to avoid surgery after a 1-year follow-up. However, athletes who played overhead sports such as tennis and baseball had less significant improvements and outcomes.
There are 3 phases of rehabilitation for those undergoing physical therapy. These phases will include:
- The acute phase: Prioritising activation of specific muscular activation. During this period, it is important to minimize stress through the injured shoulder.
- The recovery phase: Strengthening the core, specific muscle training and working the kinetic chain (movement and muscles around the injured site)
- Functional phase: Focussing on more sport-specific rehabilitation such as explosiveness, endurance, and agility.
Below will be a small sample rehabilitation programme for a baseballer suffering from a labral injury.
|
Phases |
Rehabilitation guidelines |
Example Exercises |
|---|---|---|
| Acute phase |
|
|
| Recovery Phase |
|
|
| Functional Phase |
|
Table 1. Example exercises through the 3 phases of rehabilitation. Refer to the videos in the links.
Post-surgical management
Besides stable SLAP lesions, most specialists would advocate for surgical intervention. During the surgery, the specialist will aim to re-attach the labrum back onto the shoulder socket. However, seeing a physical therapist before the surgery may help to fast-track the post-operative recovery. On the other hand, undergoing physical therapy after surgery is essential to safely progress the candidate’s recovery and return to sports.
The physical therapist will usually work with the specialist’s recommendations and the patient’s goals to tailor an appropriate exercise programme. The protocol in table 1. Is also applicable to structuring a post-operative rehabilitation plan. Importantly, the patient’s input during the rehabilitation progress is crucial to determine an optimal management plan.
Despite the complexity of labral tears, they can be managed conservatively with physical therapy where appropriate. In most cases, it is recommended to seek the advice of relevant health professionals for a faster recovery. For any further advice or support, please do not hesitate to send me an email at lmao@toptotoe.com.au.
Disclaimer: This article is not intended medical advice or a treatment plan. All content such as text, images, videos and tables in this article is for general information only. Please seek the expert opinion of a relevant health professional for any advice, diagnosis or treatment.